As with many other professions, both within and beyond the health industry, the role of a dietitian is constantly changing and diversifying into new areas in a highly changeable work environment.
Dietitians Australia has historically set standards for best practice, fostered professionalism, and provided the basis for internal disciplinary mechanisms for the protection of members and the public. This is specified in the Code of Conduct for Dietitians & Nutritionists.
This Code requires Dietitians Australia members to assume responsibility for their competence and to act with integrity and honesty, and within the limits of their qualifications and expertise.
Our Scope of Practice defines the role of an Accredited Practising Dietitian (APD) and supports decisions around practice through the use of a decision making framework. This framework guides dietitians to determine if a particular activity is within the scope of safe dietetic practice for an individual practitioner. Ethical practice demands that each practitioner is responsible for evaluating and justifying their own scope of practice.
Scope of Practice
The breadth of professional practice being carried out within the dietetic profession in Australia is expanding rapidly. In the past, most dietitians were employed in the hospital sector. Now many work in various aspects of the food and nutrition industry. Hence, the contexts in which individual dietitians work, the population groups they serve and the services they provide may be very different.
The Code of Conduct for Dietitians & Nutritionists describes the skills, knowledge, attitudes, and ethical behaviour expected of Dietitians Australia members. It does not provide a description of the level of education, experience, skill or competency required to carry out those activities. These will vary between individual providers. Within a particular practice area, individual APDs skills and knowledge will range from entry level to highly skilled.
The key purpose of the profession of dietetics is to contribute to the promotion of health and the prevention and treatment of illness by optimising the nutrition of communities and individuals. It utilises scientific principles and methods in the study of nutrition and applies these to influencing the wider environment affecting food intakes and eating behaviour.
Dietitians Australia's definition of a dietitian (2013) is:
“The profession of dietetics contributes to the promotion of health and the prevention and treatment of illness by optimising the nutrition of populations, communities and individuals. Dietitians have a defined and recognisable body of knowledge and utilise scientific principles and methods in the study of nutrition and dietetics, applying these results to influence the wider environment affecting food intake and eating behaviour. The scope of dietetic practice is such that dietitians may work in a variety of settings and have a variety of work functions.” (Approved by Dietitians Australia Board July 2013).
Evidence Based Practice International Confederation of Dietetic Associations (ICDA) further elaborates:
“Evidence-based dietetics practice is about asking questions, systematically finding research evidence, and assessing the validity, applicability and importance of that evidence. This evidence-based information is then combined with the dietitian's expertise and judgment and the clients or community’s unique values and circumstances to guide decision-making in dietetics.” (Copyright ICDA).
Definition of dietetic practice
The Dietitians Australia Board approved the following definition of dietetic practice in September 2014:
Dietetic practice includes using professional knowledge in both clinical and non-clinical relationships with patients or clients, communities and populations and can be working in management, administration, education, research, advisory, communication, program development and implementation, regulatory or policy development, food service, food security, food supply, sustainability and any other roles that impact on safe, effective delivery of services in the profession and/or using professional skills.
Dietitians Australia seeks to prepare competent graduate dietitians through a ‘generalist’ education, with a range of knowledge, skills and attributes as described in the National Competency Standards. Entry level dietetic competencies ensure all APDs have been assessed as competent in a variety of areas reflecting socio-ecological approaches to health, major health priorities and the broad landscape of dietetic practice, including policy and the provision of services and care to individuals, groups, communities and populations.
Competence encompasses meeting certain minimum requirements or standards to be able to perform the required activities of a particular profession in the workplace. Competency standards for the dietetic professional relates to the grouping of attributes, such as knowledge, attitudes and skills into manageable units for the purposes of education and assessment.
For a dietitian to develop beyond the novice stage or be able to move into a new area of practice, further education and training will be needed to expand their scope of practice. Dietetic professionals embrace the concept of lifelong learning, through continuous, self-initiated, self-directed and self-evaluated professional development, which is in parallel with many of the principles of Continuing Professional Development (CPD) and facilitated through the APD Program.
APDs are recognised professionals with the qualifications and skills to give expert nutrition and dietary advice. APDs are qualified to advise individuals and groups on nutrition related matters. APD is the only national dietetic credential recognised by the Australian Government, Medicare, the Department of Veterans Affairs and most private health funds as the quality standard for nutrition and dietetics services in Australia. It is a recognised trademark protected by law.
The APD Program is the main channel for Dietitians Australia’s CPD activities for dietitians. CPD is an integral part of being a professional. Dietitians Australia prefers the term ‘continuing professional development’ to ‘continuing professional education’ as it is seen as broader, encompassing skill and experiential learning as well as knowledge. CPD carries the individual practitioner through from novice level, through expertise, to advanced practice where judgement enhances knowledge.
The APD program has 2 credentials:
- Accredited Practising Dietitian (APD)
- Advanced Accredited Practising Dietitian (AdvAPD)
AdvAPDs are professional leaders in their field of nutrition and dietetics, with high level knowledge and skills demonstrated in 5 domains of practice:
- Leadership and influence
- Professional competence
- Research and evaluation
- Education
- Supervision and mentoring
- Strategic and reflective approach to practice.
Dietitians Australia does not classify a dietetic practitioner as a ‘specialist’. However, those practitioners who choose to specialise in a particular area of dietetics may be eligible to become an AdvAPD through the professional recognition program if they have the necessary broader skills and expertise.
Dietitians Australia's APD Role Statements acknowledge that dietitians working in specific areas can demonstrate a greater understanding and have a higher level of skill and knowledge in that particular area. The role statement can be used to promote and advocate for the unique skill, knowledge and expertise of an APD.
Extended Scope of Practice describes a discrete knowledge and skill base additional to the recognised scope of a profession and/or regulatory context of a particular jurisdiction. These would be tasks usually undertaken by other professions for example, doctors, nurses or other allied health professionals. Extending scope should be permitted where it allows more efficient management and care of the patient and decreases the number of visits or transactions in the patient journey.
For dietetics, extended scope could include tasks such as taking blood glucose levels, adjusting insulin dosages, inserting nasogastric feeding tubes and other procedures pertinent to the field of practice.
Legislative change may be required to allow extended scope of practice, for example, prescribing of drugs.
In undertaking these roles, it is expected that a practitioner has the relevant experience and the necessary credentials.7 It would be appropriate that the workplace will provide options for applicable training to ensure that the practitioner can undertake this role competently and safely. If this was permitted, clear governance would be articulated and documented policies and procedures would be available and appropriate risk management addressed.
Practitioners shall practice dietetics in this manner only to the extent that they have:
- undertaken necessary additional education and training, clinical practice supervision and support
- certification and credentialing through their workplace
- ensured that they have appropriate professional indemnity insurance cover for that practice (if in private practice, self employed)
- established and maintain their ability to work safely and competently
The following guiding principles should be used to determine scope of practice.
- The dietetic profession encourages the innovative extension of the scope of practice provided such development is based on evidence of efficacy and safety and dietitians undertake appropriate accredited training and participate in a credentialing program.
- Dietitians in Australia who have either graduated from a Dietitians Australia accredited course in Australia or passed the Dietitians Australia examination for overseas qualified dietitians, are committed to the Code of Conduct for Dietitians & Nutritionists. They can be subject to annual random audit and may be involved in disciplinary action as needed.
- An APD is committed to ongoing training and education through the APD Program requiring an annual minimum of 30 hours of professional development.
- Dietitians apply an evidence based approach to inform their scope of practice.
- Dietitians support each other through professional activities to promote dietetic practice and better food, better health and better living for all Australians.
- Dietitians and their Association seek to reduce confusion and misinformation about nutrition and clarify some of the myths surrounding nutrition for the public.
- Dietitians work towards achieving justice in the provision of nutrition and dietetic services for all people.
- Dietitians accept responsibility for all treatment provided by others acting under their supervision.
- Dietitians act in accordance with relevant legislation and seek authorisation from their employer or insurance provider if in private practice.
Summary
Dietitians Australia recognises that the role of dietitians continues to expand and does not wish to define practice too narrowly, as it may stifle innovation. It also recognises that there are several models of nutrition and dietetic services provision that can be implemented to ensure equity of access to dietetic services in a cost effective manner. Whatever the model of nutrition and dietetic service provision, there needs to be recognition of the distinct roles that dietitians and non-dietitians have in the provision of these services. Ultimately, dietitians shall accept responsibility for all interventions provided under their management 5.
The Scope of Practice Decision Tool (below) is a framework for practitioners to assess whether a task is a core or extended activity for an APD. It also provides guidance for practitioners to extend scope of practice safely and ethically.
Scope of Practice Decision Tool
Follow the questions in the decision tool to assess the practice.
- If you answer yes to each of the questions, you are competent to perform the activity as required in accordance with organisational policies and procedures
- If you have not answered yes to each of the questions, DO NOT PROCEED UNTIL DECISION POINT IS RESOLVED
- If it is not in line with the Code of Conduct or if you do not accept responsibility and accountability for the action then you should not continue
- The guiding questions are to assist you as you use the decision tool
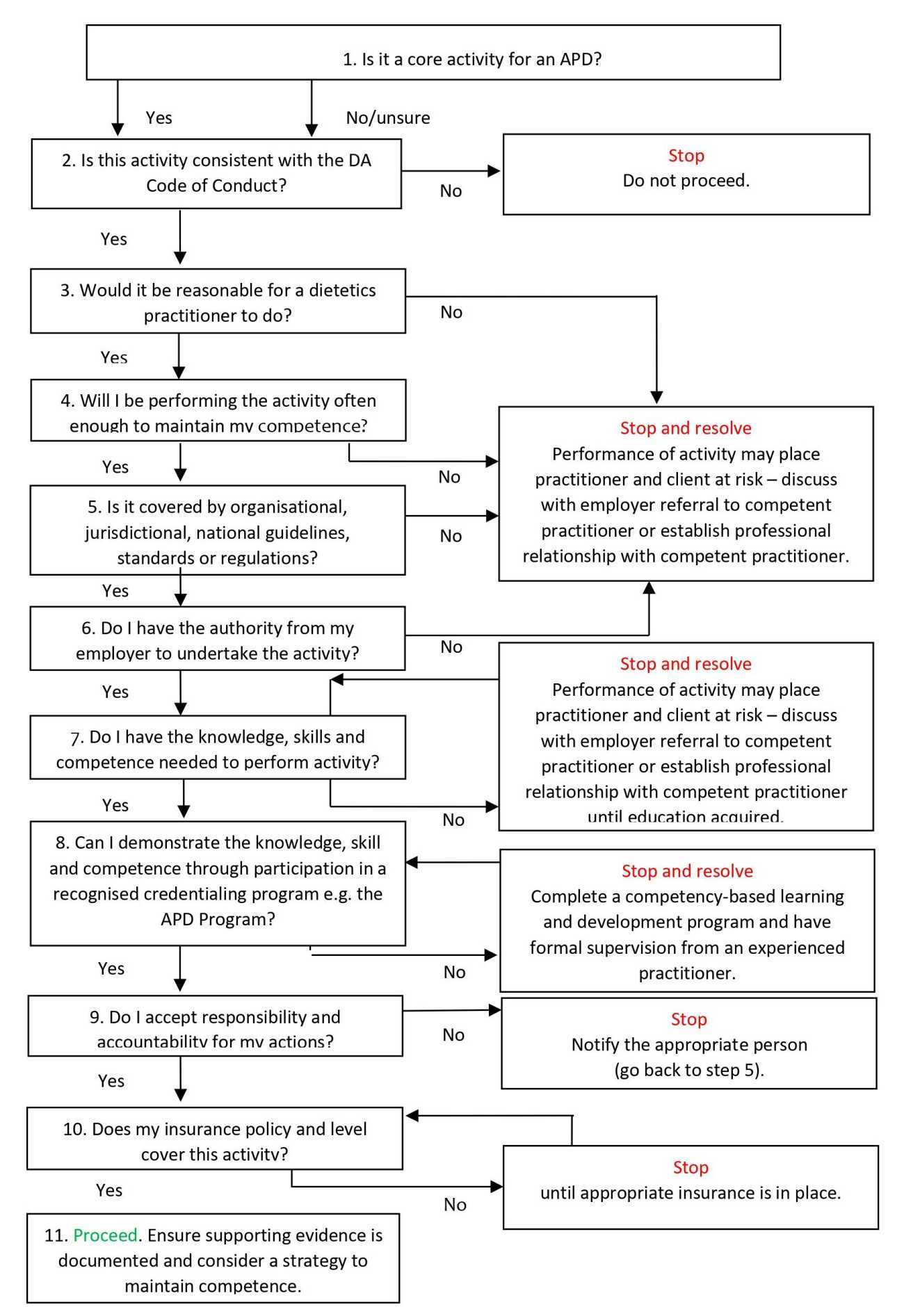
The decision tool was adapted from the American Dietetic Association: Scope of Dietetic Practice Framework.1
Guiding questions for the use of the Decision Tree
If you answer yes to each of the questions, you are competent to perform the activity as required in accordance with organisational policies and procedures. If you haven't answered yes to each of the questions, DO NOT PROCEED UNTIL DECISION POINT IS RESOLVED.
1. Is it a core activity for an APD? Is the activity covered by the National Competency Standards?
2. Is this activity consistent with the Code of Conduct for Dietitians & Nutritionists? If the answer is no then the activity should not be considered.
3. Would it be reasonable for a dietetics practitioner to do? Is the activity covered by the National Competency Standards? Would the activity be within the accepted ‘standard of practice’ that would be provided in similar circumstances by an APD who has similar training, education, skill, competence and experience?
4. Will I be performing the activity or service often enough to maintain my skills and competence? Will I be undertaking on a regular basis?
5. Is the activity covered by organisational, jurisdiction, National or guidelines, standards or legislation? For example,
- institution job descriptions
- organisation accrediting/credentialing standards
- nutrition or dietetic practice guidelines
- jurisdiction or federal legislation or regulations
6. Do I have authority from my employer? Is the activity or service consistent with my job description? Has my employer provided authority for me to undertake this activity? (If a private practitioner is self-employed, then they are also the employer). Do I have the education and training needed, professional supervision in place, ongoing CPD and assessment, agreement with from the rest of the multi disciplinary team and workplace and/or checked with insurance policy (if applicable)? Ensure you have written evidence of education, training, assessment and supervision is available.
7. Do I have the knowledge, skills and demonstrated competence needed? Have I acquired the depth and/or breadth of knowledge, skills and competence needed to safely and effectively perform this activity or service through recognised accredited training, such as a pre-professional program, a CPD program, self-study or mentoring with a more competent practitioner?
8. Have I personally demonstrated current knowledge, skills and competence to safely perform this activity or service for example, via the APD program or an equivalent credentialing program?
9. Do I accept responsibility and accountability for my actions? Am I personally prepared to accept the consequences of my actions or do I need to discuss this further with my employer?
10. Does my current insurance policy and level cover this activity? Am I covered by my employer’s or my personal professional indemnity insurance or do I need to increase the level my insurance or take out an additional policy to cover this specific activity? The box should reflect ‘does my employer indemnify me?’
11. Proceed if supporting evidence is documented and consider a strategy to maintain competence. Do I have supporting evidence regarding the relevant decision points which is updated regularly as required, for example, qualifications, certificate of registration/attainment, statement in policy and procedure manual, supporting correspondence from employer/practice manager, membership of credentialing organisation?
- Case study 1
-
An APD has been recently appointed to a senior clinician position in a large metropolitan tertiary hospital. The APD has been referred to a patient with Motor Neurone Disease who is enterally fed via gastrostomy. The referral is requesting nutrition review and PEG change. Would this work role be within the APDs scope of practice?
1. Is it a core activity for an APD? YES, for nutrition review but NO for PEG change.
2. Is this activity consistent with the ‘Code of Conduct for Dietitians & Nutritionists’? YES
3. Would it be reasonable for a dietetic practitioner to do? YES
4. Will I be performing the activity or service often enough to maintain my skills and competence? YES, as part of PEG care team.
5. Is it covered by any organisational, jurisdiction or national or guidelines, standards or regulations/legislation? This is not within a regulatory framework, the practice has been approved by the organisation’s credentialing process at that hospital, and there are no national practice guidelines.
6. Do I have authority from my employer to undertake this activity? YES, this practice has been credentialed at this hospital; it is included in job description.
7. Do I have the knowledge, skills and demonstrated competence to undertake this activity? NO, not yet but my employer is putting me through a competency based training program to credential for this skill (PEG change).
8. Can I demonstrate knowledge, skills and competence through participation in a recognised credentialing program? YES, APD completed learning program or course supported by employer and undertook supervised practice.
9. Do I accept responsibility and accountability for my actions? YES
10. Does my current insurance policy and level cover this activity? YES, covered by hospitals insurance policy and this employer as it is an agreed activity for dietitians in this hospital. If you transferred to another hospital you would need to check whether this is accepted credentialed practice in that hospital.
11. Proceed as supporting evidence is documented. Consider a strategy to maintain competence with your manager and as part of your APD program.
- Case study 2
-
An APD is employed in a rural community health centre. The APD’s colleague leaves and the APD has been asked to cover the paediatric clinic for 3 months by the services manager. The APD has no post-entry level work experience in paediatrics. The first patient she/he is asked to see is a 2-year-old with food allergy. Would this work role be within the APDs scope of practice?
1. Is it a core activity for an APD? YES
2. Is this activity consistent with the Code of Conduct for Dietitians & Nutritionists? YES
3. Would it be reasonable for a dietetic practitioner to do? YES
4. Will I be performing the activity or service often enough to maintain my skills and competence? NO, but discussed with supervisor and has developed strategies to address this issue, including mentoring and support from dietitian with experience in paediatrics in a regional centre.
5. Is it covered by any organisational, jurisdiction or national or guidelines, standards or regulations/legislation? YES, job description as responsible for dietetic care.
6. Do I have authority from my employer to undertake this activity? YES, part of job description as APD
7. Do I have the knowledge, skills and demonstrated competence to undertake this activity? YES, while the APD may feel that she/he has not experienced these types of patients before, the entry-level qualification prepares the APD adequately to work with paediatric patients.
8. Can I demonstrate knowledge, skills and competence through participation in a recognised credentialing program? YES, as an APD
9. Do I accept responsibility and accountability for my actions? YES
10. Does my current insurance policy and level cover this activity? YES, covered by workplace insurance policy
11. Proceed as supporting evidence is documented and consider a strategy to maintain competence. The APD may consider CPD activities related to paediatric nutrition to increase knowledge, skills and confidence win working in this area. For example, obtain a mentor, enrol in a short course.
- Case study 3
-
An APD has recently completed a Diploma of Naturopathy in addition to the entry level dietetic training and they wish to incorporate this into their dietetic practice by recommending and selling supplements as part of management of patients with type2 DM. Would this work role be within the APDs scope of practice?
1. Is it a core activity for an APD? NO, seeing the patient with diabetes is core activity, but incorporation of supplements in this case is not evidence based practice.
2. Is this activity consistent with the Code of Conduct for Dietitians & Nutritionists? NO, if the APD wishes to practice naturopathy then they must make it clear to the client and their health care team that is what they are practicing and that they are not practising dietetics, STOP do not continue to see patients until the practitioner decides whether to continue to identify as a dietitian
- References
-
- O’Sullivan Maillet J, Skates J & Pritchett E. 2005,’ American Dietetic Association: Scope of Dietetics Practice Framework’ Journal of the American Dietetic Association, vol. 105, no. 4, pp. 634-640.
- Dietitians Australia. Constitution and By-Laws
- International Confederation of Dietetic Associations. Evidence-based dietetics practice. ICDA, 2013 Available from http://www.internationaldietetics.org/Downloads/ICDA-Standard-Evidence-based-Dietetics-Practice.aspx
- Dietitians Australia. National Competency Standards.
- The APD Handbook https://member.dietitiansaustralia.org.au/apdhandbook
- Dietitians Australia. Role Statements.
- The Academy Quality Management Committee and Scope of Practice Subcommittee of the Quality Management Committee. Academy of Nutrition and Dietetics: Scope of Practice in Nutrition and Nutrition and Dietetics Journal of the Academy of Nutrition and Dietetics: June 2013, vol 133, No 6, S11-16.