As the leading voice in nutrition and dietetics, we're helping build healthy communities. Read our advice to learn how diet and nutrition can improve your health and wellbeing.
Evidence-based health advice
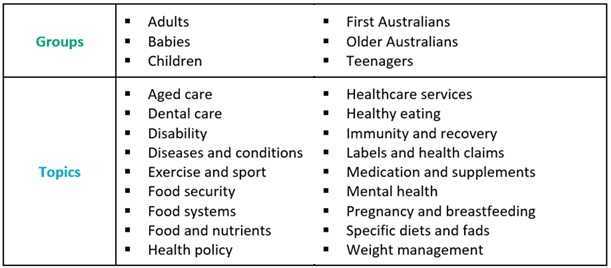
Our growing library of health advice articles feature the latest scientific evidence about human nutrition. Our Interest Groups and Accredited Practising Dietitians inform the health advice we give to you.
Smart eating advice
We'll answer your diet and nutrition questions and help you understand how to eat smarter. You'll learn nutrition facts and how your diet can help you manage your health.
When to see a dietitian
We'll help you understand when you need to see a dietitian. A dietitian can give you personalised advice and a healthy eating plan specific to your nutritional needs.
Use our online search tool to find a dietitian.
Get in touch
We'll be adding more health advice articles to our website over the coming months. If you have questions about our health advice, contact us at info@dietitiansaustralia.org.au
Library of Health Articles